Hip Op Hooray or Hip Op No Way!
Posted on 14th January 2020 at 09:52
Happy New Year folks and what better way to start 2020 than with a hip new blog! Following hot on the heels of the film "Resurfacing", documenting the trials and tribulations of Andy Murray overcoming his hip problem and his successful return to professional tennis, Gary Jones, Clinic Director at PHYSIO 206 discusses the why, what and when of common types of hip surgery.
Hip and groin pain is a common problem we see affecting all generations of life. There can be multiple reasons for this, such as slipped femoral epiphysis (S.U.F.E) in children (which I must add does require immediate surgical intervention), referred pain from the lower back and pelvis as well as soft tissue injuries including groin strains and tendon issues. However, the most common cause of groin pain is actually related to an issue affecting the hip joint and in particular the cartilage that lines the surface of the joint. This is often referred to as "Arthritis", "Wear and Tear" or "Age Related Change".
In the case of osteoarthritis, the conundrum that many orthopaedic surgeons face and the challenges this poses to you the patient as well as the treating physiotherapist could be demonstrated no more clearly than in the case of Andy Murray and his announcement that he was considering retirement from professional tennis due to his persistent hip pain caused by his arthritic hip. He wanted a better quality of life and having a partial joint replacement in the form of a hip resurfacing was the solution that he sought.
Yes you did hear that correctly! A partial joint replacement! Essentially, Andy Murray has an arthritic hip at the age of 32. No offence intended but when people start thinking about joint replacement we are generally talking from the age of 50 plus. He's certainly got a good few years to go there and this is where the management of people, such as Andy (we are not personal friends by the way), who have pain related to cartilage loss at the joint becomes more tricky. Whether that's a hip, knee or ankle joint the options out there to patient's are not the golden panacea.
So, why do people develop symptoms in relation to Osteoarthritis from an early age. There is lots of debate and conjecture around this subject. Essentially if you were to x-ray or scan anyone's hips from the age of 30/35 onward you are likely to see some changes in the cartilage that lines the surface of the joints. This applies to all joints. However, not everyone will experience pain. The following reasons have been suggested for developing osteoarthritis at an early age:
Genetics - In other words "blame you parents!" A family history of joint replacement is often reported.
Trauma - If you have had a fracture or sustained some bone bruising this can lead to the earlier onset of arthritis.
Congenital reasons - Another one to thank the folks for! Essentially some people are born with a hip joint that is a certain shape that can pre-dispose them to the early onset of osteoarthritis.
Females that are post menopausal.
Occupational and recreational activities - This is a more tenuous link as we see equal amounts of people that lead very active lifestyles and sedentary lives that require joint replacement.
There has also been some suggestion that certain lifestyle factors can impact on the quality of the cartilage that lines the surface of your joints. These include things such as a high body mass index (i.e being overweight can cause increased pressure on the joints), smoking and nutritional deficiencies.
One of the main reasons cited for developing Osteoarthritis in the hip over recent years is a condition called hip impingement.
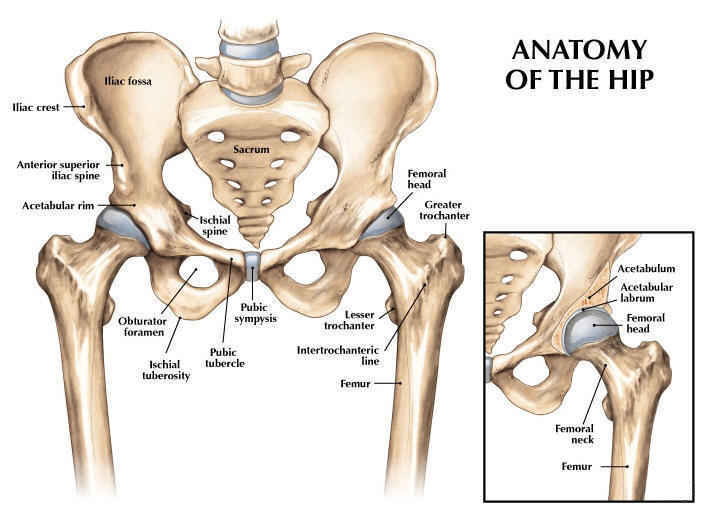
Hip impingement (Femoroacetabular impingement otherwise known as FAI) is a condition involving one or more anatomical abnormalities of the hip joint. It is common in people that play hockey tennis and football as well as equestrianism and is more common in younger males than females. It occurs when the ball shaped head of the thigh bone (femur) contacts the hip socket (acetabulum) abnormally or does not permit a normal range of motion in the acetabular socket. There are 3 types of hip impingement:
1. Cam Impingement - An excess of bone (a Cam) along the upper surface of the femoral head (the ball part of the joint). This is the type of impingement that is most likely to lead to the development of Osteoarthritis in the hip joint.
2. Pincer Impingement - An excess of growth of the upper lip (a pincer) of the acetabular cup (the socket part of the joint)
3. Mixed impingement - The most common type. 70% of all hip impingement presentations are characterised by a combination of cam and pincer defects.
Hip impingement can lead to inflammation of the joint, surrounding soft tissues and impact on the cartilage ring that lines the surface of the socket of the hip joint (the Labrum). Clinically, pain is often felt in the groin but may also extend into the buttock and lower back.
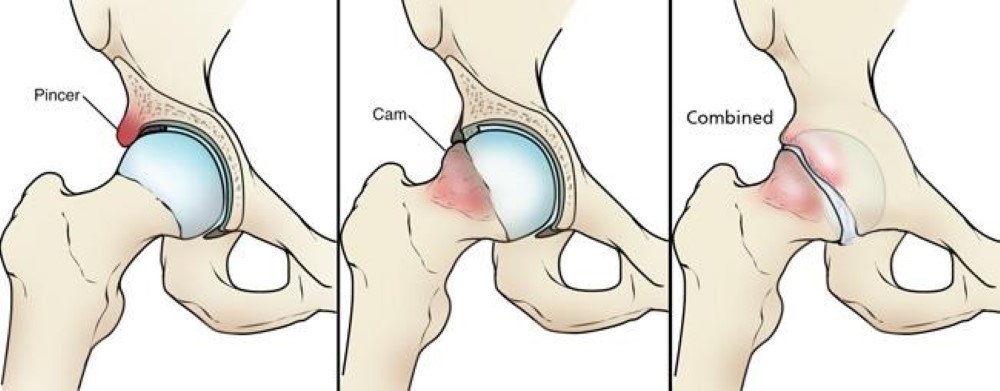
Types of Hip Impingement
Some of the early warning signs for this are pain and/or limited range of motion at the hip when trying to put socks/shoes on, pain in the hip and groin if performing squats and also getting in/out of the car. A very simple clinical test called the FADIR test (Flexion ADuction Internal Rotation) which involves bending the hip and rotating inwards/across the body is often used by Physiotherapists to make a clinical diagnosis in combination with the Fabers test (taking the hip outwards with the hip and knee in a figure 4 position). This then needs to be correlated with further investigations in the form of X-rays and/or MRI imaging.
So what are the options in terms of treatment for the management of an arthritic hip in a young adult.
1. Conservative Management
This essentially means getting the best out of your hip joint in terms of function without having operative intervention. This is such an important part of the management process and needs to be done with an holistic outlook and is strongly recommended before going down the operative route. Andy Murray certainly tried this for several months before accepting that there was no other option.
Physiotherapy can be of great help with this condition and a combined approach to treatment is advocated. This would comprised of manual therapy (hands-on treatment) to help improve the mobility of the soft tissues at the hip joint and other joints around it and exercise based rehabilitation. This is the key bit and the thing that will help provide a more longer term solution to your symptoms. Bespoke exercise based rehabilitation that improves muscle control, strength and flexibility as well as focusing on addressing any biomechanical or postural issues that could be impacting on someone's hip function is key. Looking at how the body as a whole impacts on hip loading is key, whether a sports person or not.
Injection therapy, in the form of a steroid and local anaesthetic can be very helpful in conjunction with a good rehabilitation programme. There is little evidence to support the effectiveness of acupuncture, taping or electrotherapy modalities for this issue.
2. Surgical Management
A) Hip Arthroscopy
This can be an effective procedure when treating a young arthritic hip, especially in the case of hip impingement. 2-3 very small incisions are made and through the process of keyhole surgery, small instruments are used to help smoothen joint surfaces, remove pieces of excess bone and to help repair the ring of cartilage in the hip socket (the labrum) if necessary.
Outcomes are generally good, as long as there is good compliance with the rehabilitation programme set and return to sport is often the reason for this surgery. Recovery can take 3-6 months but is some cases 9-12 months dependent on the work that is required.
B) Hip Resurfacing
The procedure that Andy Murray underwent (the film titles a give away really!) . As a Brummy, I am proud to say that this was developed right here in our great city, Birmingham!
Again a very good operation that yields good outcomes. This procedure involves partial replacement of both the hip socket and the ball of the ball and socket joint too. Not as much bone removed as a total hip replacement and with a smaller prosthesis too, therefore recovery time is quicker. In my experience, clients with often return to sport in 6-9 months though on occasions this process can take 12 months. Return to tennis and skiing are common sports that people return to after this surgery.
C) Hip Replacement
Generally, the final solution for managing a young arthritic hip and most commonly used for the management of the older arthritic hip. This would be the surgery of choice if the above options are not suitable for the individual in question, if the individual needs to convert from a hip resurfacing to a full replacement or if the joint is significantly worn.
Again the outcomes following a hip replacement are very good. Firstly, from a pain relief perspective and also from a functional perspective with clients I have worked with returning to recreational tennis and skiing. With the advances in surgical techniques and in the types of prosthesis now used, it is not uncommon for a hip replacement to survive a 15-20 year time frame. Rehabilitation can take 9-12 months to achieve the desired outcome.
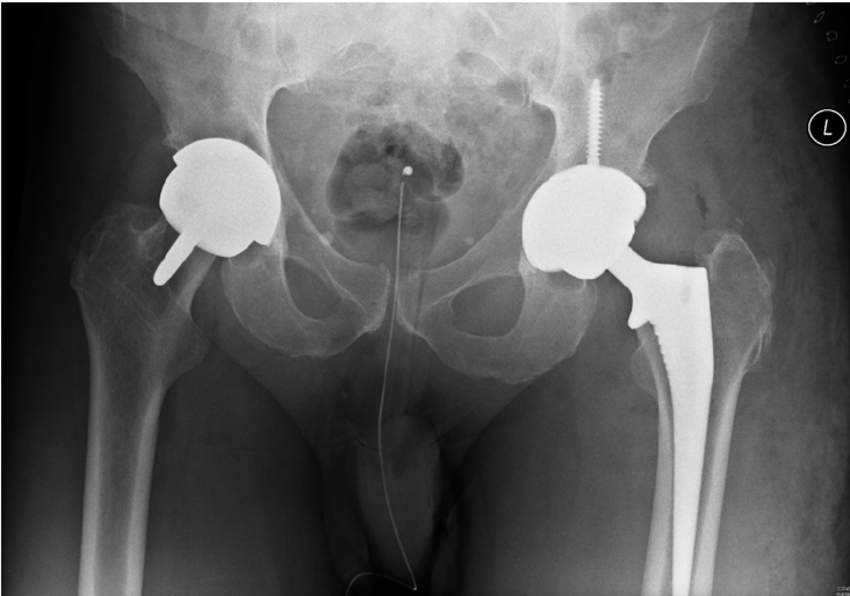
Hip Resurfacing (Right)
Vs
Hip Replacement (Left)
So, if you are experiencing hip and groin pain, dont suffer in silence. Speak to an experienced physiotherapist.
You can see from this post that there are a number of options available to help manage this problem. If you would like to know more about the role that physiotherapy can play in this process then do not hesitate to get in touch. Andy Murray with real grit, determination, motivation and commitment to the rehabilitation process has got back to where he wants to be. If you would like to get back on that tennis court, football pitch, back on to your horse or quite simply be able to put your socks and shoes on with less pain then get in touch. We'd be delighted to help you to achieve what you want to do.
Share this post: